Here's the View from my Knothole
The number of COVID-19 cases continues to increase, in part due to recent holiday gatherings; new more contagious strains; and exhaustion with social distancing.
We are nearing completion of 365 days of unprecedented chaos, at least for me. Although experts in infectious disease have been thinking about and planning for an infectious disease outbreak of such magnitude, many—myself included—had no expectation of it in our lifetime. Measures to stall the spread of coronavirus disease 2019 (COVID-19) and the ensuing social isolation have transformed the workplace, school, and home environments.
The availability of a COVID-19 vaccine has been touted as the start of the return to normal. Once the population is vaccinated and immunity is prevalent, we can anticipate life returning to something closer to what we once knew. That said, I recognize that the definition of “normal” will be different than how I would have described it a year ago.
The number of COVID-19 cases continues to increase (Figure), in part due to recent holiday gatherings; new, more contagious strains of the COVID-19 virus; and exhaustion with social distancing. The strain of needing to continue isolation, wear masks, be diligent about hygiene has taken a toll. We must continually remind ourselves and others to stay socially distant in break rooms, not eat together, and remain vigilant.
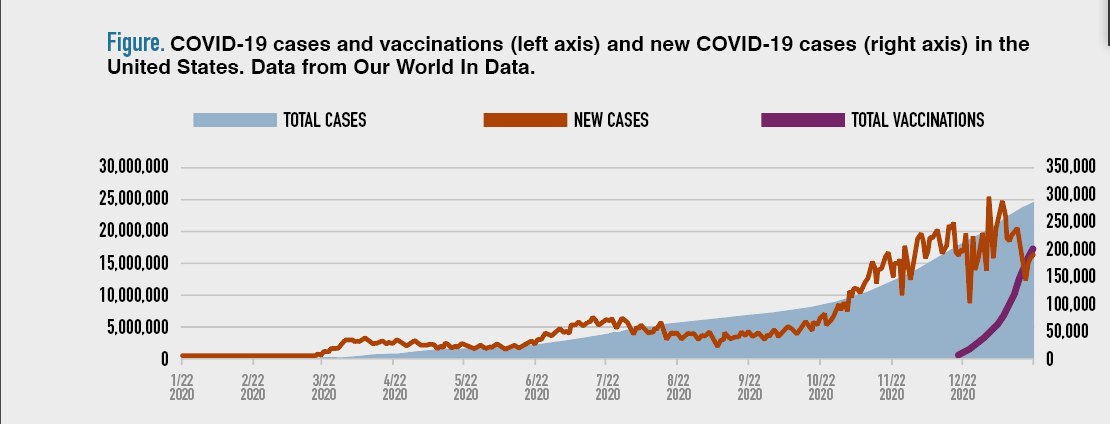
The vaccine now has been rolled out via different strategies in each state, yet the uptake is not as robust as hoped. Vaccine rollout has been challenging, with facilities wanting to protect the most vulnerable and ensure it is performed with the requisite social distancing. As we move to encourage vaccination, with the hope that this will stall spread, numerous questions and concerns are raised about the vaccine. Importantly, these concerns are not just among the lay public—many providers and hospital personnel also have questions and concerns. If health care workers, who clearly have seen the devastation of this virus, are not willing to accept vaccination, it will be difficult to sway the lay public.
Many of the concerns swirl on social media: “Will the vaccine impact fertility, hair growth or loss, or onset of Bell’s palsy?” Some have a grounding in the trials that led to the vaccine’s approval, and others seemingly appear without any basis in fact. In this issue of Contemporary OB/GYN®, Emily Adhikari, MD, medical director of Perinatal Infectious Diseases at Parkland Health and Hospital System and an assistant professor of obstetrics and gynecology at the University of Texas Southwestern Medical Center in Dallas, addresses these frequently asked questions. She has created a tear-out for our Well Woman section, also available for download online, for your practice guidance.
We all need to understand the facts about vaccination; be role models of hygiene, masking, and social distancing; and talk with our coworkers, practitioners, family, and friends to address their questions about vaccination.
I sometimes wonder if I am having a nightmare and will wake up to find all is well with the world, only to realize that it is all too true. Recognizing that others, less informed than we are, also may be experiencing the same thoughts means that we must continue to offer hope and encouragement to our coworkers, patients, friends, and communities. Please stay strong and stand tall!

Impact of antiepileptic medications and sex hormones on maternal and child outcomes in epilepsy
May 16th 2024Paula Emanuela Voinescu, MD, PhD, director of the Women's Epilepsy Program at Brigham and Women's Hospital, talked about the influence of sex hormones on maternal outcomes in pregnant women with epilepsy treated with antiseizure medication.
Read More
PCOS and irregular cycles tied to cardiometabolic risks
May 15th 2024A comprehensive analysis reveals strong associations between polycystic ovary syndrome, irregular menstrual cycles, and increased risks of cardiometabolic conditions, underscoring the importance of proactive screening and intervention strategies.
Read More
Impact of primary care physicians on cervical cancer screening disparities
May 14th 2024A study highlights how having a primary care physician significantly increases the likelihood of cervical cancer screening among lesbian, gay, and bisexual cisgender women, addressing disparities exacerbated by systemic discrimination and healthcare access challenges.
Read More
Unlocking HPV prevention: Insights from 2022 data on vaccination trends
May 14th 2024Explore the latest findings revealing vaccination rates among children aged 9 to 17 years, uncovering demographic disparities and highlighting the crucial role of vaccination in combating human papillomavirus infections and related health risks.
Read More
